Search
- Page Path
- HOME > Search
- Miscellaneous
- AM1638, a GPR40-Full Agonist, Inhibited Palmitate- Induced ROS Production and Endoplasmic Reticulum Stress, Enhancing HUVEC Viability in an NRF2-Dependent Manner
- Hwan-Jin Hwang, Joo Won Kim, SukHwan Yun, Min Jeong Park, Eyun Song, Sooyeon Jang, Ahreum Jang, Kyung Mook Choi, Sei Hyun Baik, Hye Jin Yoo
- Endocrinol Metab. 2023;38(6):760-769. Published online November 2, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1774

- 1,202 View
- 85 Download
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
G protein-coupled receptor 40 (GPR40) is a key molecule in diabetes and fatty liver, but its role in endothelial dysfunction remains unclear. Our objective in this study was to determine whether GPR40 agonists protect endothelial cells against palmitatemediated oxidative stress.
Methods
Human umbilical vein endothelial cells (HUVECs) were used to investigate effects of various GPR40 agonists on vascular endothelium.
Results
In HUVECs, AM1638, a GPR40-full agonist, enhanced nuclear factor erythroid 2–related factor 2 (NRF2) translocation to the nucleus and heme oxygenase-1 (HO-1) expression, which blocked palmitate-induced superoxide production. Those antioxidant effects were not detected after treatment with LY2922470 or TAK875, GPR40-partial agonists, suggesting that GPR40 regulates reactive oxygen species (ROS) removal in a ligand-dependent manner. We also found that palmitate-induced CCAAT/enhancer‐binding protein homologous protein expression; X-box binding protein-1 splicing, nuclear condensation, and fragmentation; and caspase-3 cleavage were all blocked in an NRF2-dependent manner after AM1638 treatment. Both LY2922470 and TAK875 also improved cell viability independent of the NRF2/ROS pathway by reducing palmitate-mediated endoplasmic reticulum stress and nuclear damage. GPR40 agonists thus have beneficial effects against palmitate in HUVECs. In particular, AM1638 reduced palmitate-induced superoxide production and cytotoxicity in an NRF2/HO-1 dependent manner.
Conclusion
GPR40 could be developed as a good therapeutic target to prevent or treat cardiovascular diseases such as atherosclerosis.

- Diabetes, Obesity and Metabolism
- Sleep Duration and the Risk of Type 2 Diabetes: A Community-Based Cohort Study with a 16-Year Follow-up
- Da Young Lee, Inha Jung, So Young Park, Ji Hee Yu, Ji A Seo, Kyeong Jin Kim, Nam Hoon Kim, Hye Jin Yoo, Sin Gon Kim, Kyung Mook Choi, Sei Hyun Baik, Seung Ku Lee, Chol Shin, Nan Hee Kim
- Endocrinol Metab. 2023;38(1):146-155. Published online February 6, 2023
- DOI: https://doi.org/10.3803/EnM.2022.1582

- 2,628 View
- 165 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
We aimed to investigate the moderating effects of obesity, age, and sex on the association between sleep duration and the development of diabetes in Asians.
Methods
We analyzed data from a cohort of the Korean Genome and Epidemiology Study conducted from 2001 to 2020. After excluding shift workers and those with diabetes at baseline, 7,407 participants were stratified into three groups according to sleep duration: ≤5 hours/night, >5 to 7 hours/night (reference), and >7 hours/night. The Cox proportional hazards analyses were used to calculate the hazard ratios (HRs) and 95% confidence intervals (CIs) for incident type 2 diabetes mellitus (T2DM). Subgroup analyses were performed according to obesity, age, and sex.
Results
During 16 years of follow-up, 2,024 cases of T2DM were identified. Individuals who slept ≤5 h/night had a higher risk of incident diabetes than the reference group (HR, 1.17; 95% CI, 1.02 to 1.33). The subgroup analysis observed a valid interaction with sleep duration only for obesity. A higher risk of T2DM was observed in the ≤5 hours/night group in non-obese individuals, men, and those aged <60 years, and in the >7 hours/night group in obese individuals (HRs were 1.34 [95% CI, 1.11 to 1.61], 1.22 [95% CI, 1 to 1.49], and 1.18 [95% CI, 1.01 to 1.39], respectively).
Conclusion
This study confirmed the effect of sleep deprivation on the risk of T2DM throughout the 16-year follow-up period. This impact was confined to non-obese or young individuals and men. We observed a significant interaction between sleep duration and obesity. -
Citations
Citations to this article as recorded by- Attention to Innate Circadian Rhythm and the Impact of Its Disruption on Diabetes
Da Young Lee, Inha Jung, So Young Park, Ji Hee Yu, Ji A Seo, Kyeong Jin Kim, Nam Hoon Kim, Hye Jin Yoo, Sin Gon Kim, Kyung Mook Choi, Sei Hyun Baik, Nan Hee Kim
Diabetes & Metabolism Journal.2024; 48(1): 37. CrossRef - Role of Sleep and Sleep Disorders in Cardiometabolic Risk: a Review and Update
Shaden O. Qasrawi, Ahmed S. BaHammam
Current Sleep Medicine Reports.2024; 10(1): 34. CrossRef - Evaluating reliability in wearable devices for sleep staging
Vera Birrer, Mohamed Elgendi, Olivier Lambercy, Carlo Menon
npj Digital Medicine.2024;[Epub] CrossRef - All That Glitters Is Not Gold: The Same Sleep Time, but Different Diabetogenic Outcomes
Bohye Kim, Obin Kwon
Endocrinology and Metabolism.2023; 38(1): 78. CrossRef - The Link Between Sleeping and Type 2 Diabetes: A Systematic Review
Ali Darraj
Cureus.2023;[Epub] CrossRef
- Attention to Innate Circadian Rhythm and the Impact of Its Disruption on Diabetes

- Diabetes, Obesity and Metabolism
- Sestrin2 Regulates Beneficial β3-Adrenergic Receptor-Mediated Effects Observed in Inguinal White Adipose Tissue and Soleus Muscle
- Min Jeong Park, Joo Won Kim, Eun Roh, Kyung Mook Choi, Sei Hyun Baik, Hwan-Jin Hwang, Hye Jin Yoo
- Endocrinol Metab. 2022;37(3):552-557. Published online June 29, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1421
- 2,639 View
- 107 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
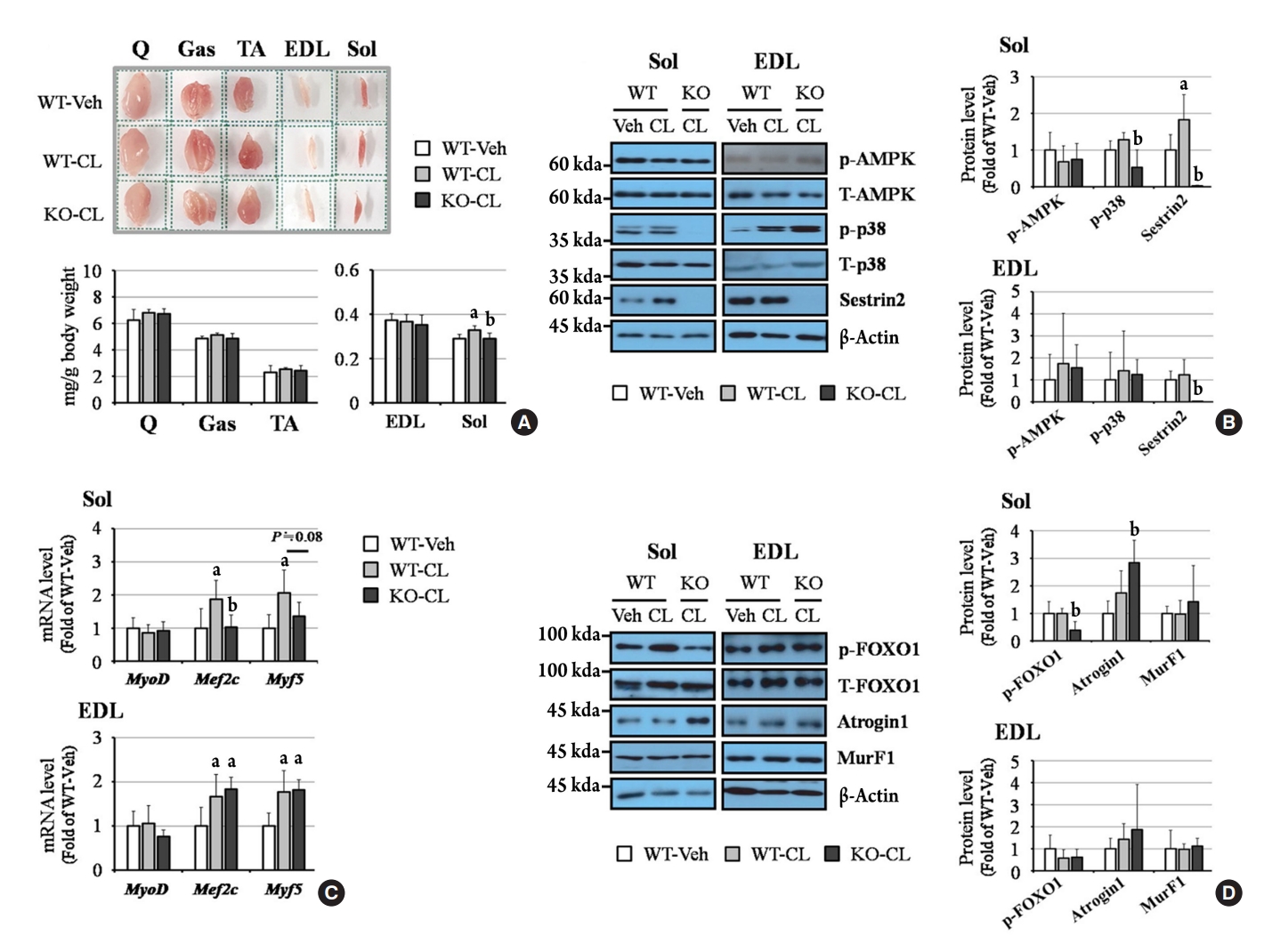
ePub - Sestrin2, a well-known adenosine monophosphate-activated protein kinase (AMPK) regulator, plays a protective role against metabolic stress. The β3-adrenergic receptor (β3AR) induces fat browning and inhibits muscle atrophy in an AMPK-dependent manner. However, no prior research has examined the relationship of sestrin2 with β3AR in body composition changes. In this study, CL 316,243 (CL), a β3AR agonist, was administered to wild-type and sestrin2-knockout (KO) mice for 2 weeks, and fat and muscle tissues were harvested. CL induced AMPK phosphorylation, expression of brown-fat markers, and mitochondrial biogenesis, which resulted in the reduction of lipid droplet size in inguinal white adipose tissue (iWAT). These effects were not observed in sestrin2-KO mice. In CL-treated soleus muscle, sestrin2-KO was related to decreased myogenic gene expression and increased levels of muscle atrophy-related molecules. Our results suggest that sestrin2 is associated with beneficial β3AR-mediated changes in body composition, especially in iWAT and in the soleus.
-
Citations
Citations to this article as recorded by- Sestrin2 levels in patients with anxiety and depression myocardial infarction was up-regulated and suppressed inflammation and ferroptosis by LKB1-mediated AMPK activation
Yufeng Qian, Lian Chen, Beibei Gao, Xianhua Ye
Clinical and Experimental Hypertension.2023;[Epub] CrossRef - Sestrin2 in diabetes and diabetic complications
Xiaodan Zhang, Zirui Luo, Jiahong Li, Yaxuan Lin, Yu Li, Wangen Li
Frontiers in Endocrinology.2023;[Epub] CrossRef
- Sestrin2 levels in patients with anxiety and depression myocardial infarction was up-regulated and suppressed inflammation and ferroptosis by LKB1-mediated AMPK activation

- Thyroid
Big Data Articles (National Health Insurance Service Database) - Risk of Diabetes in Patients with Long-Standing Graves’ Disease: A Longitudinal Study
- Eyun Song, Min Ji Koo, Eunjin Noh, Soon Young Hwang, Min Jeong Park, Jung A Kim, Eun Roh, Kyung Mook Choi, Sei Hyun Baik, Geum Joon Cho, Hye Jin Yoo
- Endocrinol Metab. 2021;36(6):1277-1286. Published online December 16, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1251
- 5,184 View
- 181 Download
- 9 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
The detrimental effects of excessive thyroid hormone on glucose metabolism have been widely investigated. However, the risk of diabetes in patients with long-standing hyperthyroidism, especially according to treatment modality, remains uncertain, with few longitudinal studies.
Methods
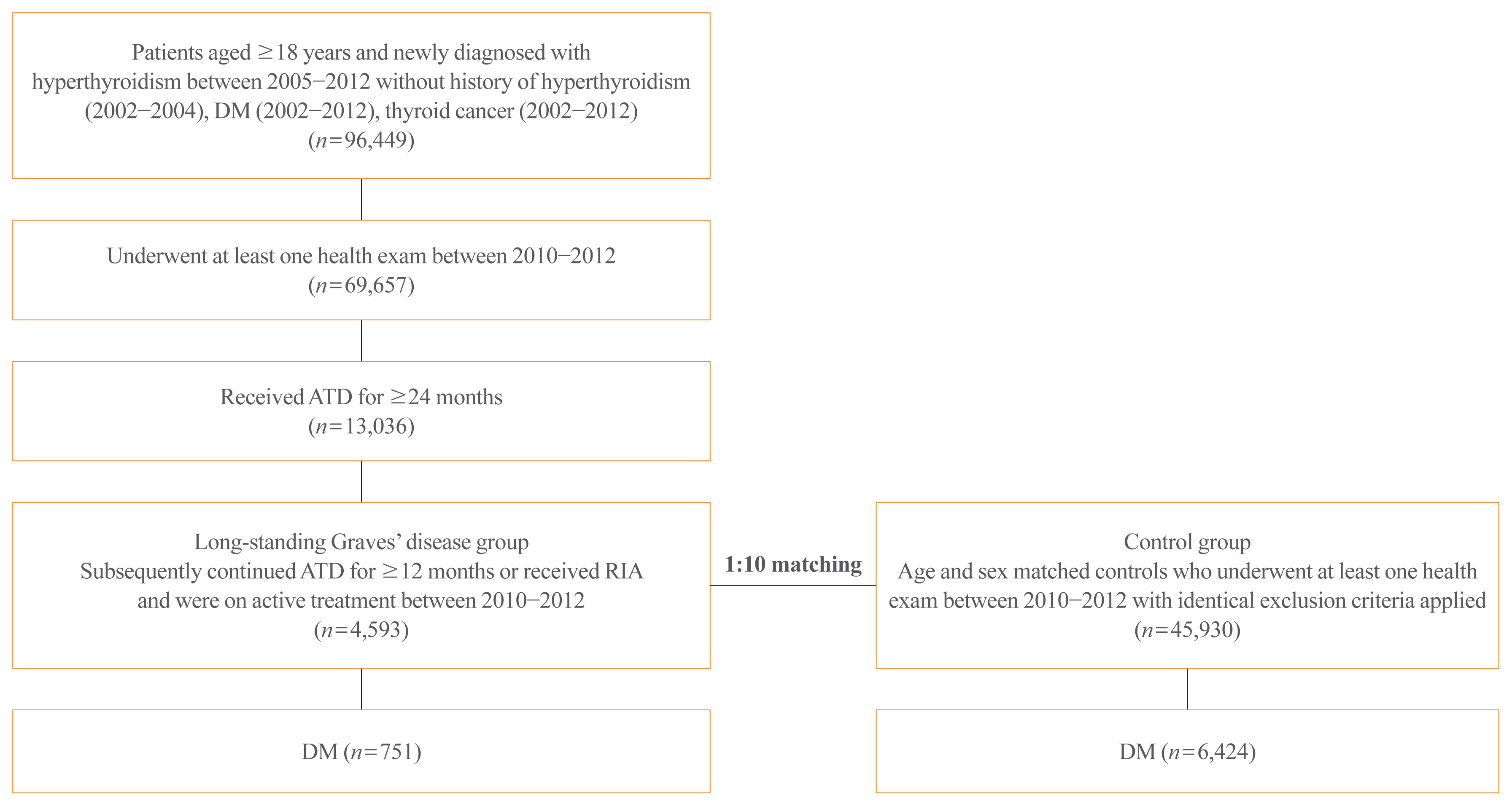
The risk of diabetes in patients with Graves’ disease treated with antithyroid drugs (ATDs) for longer than the conventional duration (≥2 years) was compared with that in age-and sex-matched controls. The risk was further compared according to subsequent treatment modalities after a 24-month course of ATD: continuation of ATD (ATD group) vs. radioactive iodine ablation (RIA) group.
Results
A total of 4,593 patients were included. Diabetes was diagnosed in 751 (16.3%) patients over a follow-up of 7.3 years. The hazard ratio (HR) for diabetes, after adjusting for various known risk factors, was 1.18 (95% confidence interval [CI], 1.10 to 1.28) in patients with hyperthyroidism. Among the treatment modality groups, the RIA group (n=102) had a higher risk of diabetes than the ATD group (n=4,491) with HR of 1.56 (95% CI, 1.01 to 2.42). Further, the risk of diabetes increased with an increase in the ATD treatment duration (P for trend=0.019).
Conclusion
The risk of diabetes was significantly higher in patients with long-standing Graves’ disease than in the general population, especially in patients who underwent RIA and prolonged ATD treatment. Special attention to hyperglycemia during follow-up along with effective control of hyperthyroidism may be necessary to reduce the risk of diabetes in these patients. -
Citations
Citations to this article as recorded by- Safety of non-standard regimen of systemic steroid therapy in patients with Graves’ orbitopathy: a single-centre experience
Nadia Sawicka-Gutaj, Dawid Gruszczyński, Natalia Zawalna, Kacper Nijakowski, Agnieszka Skiba, Mateusz Pochylski, Jerzy Sowiński, Marek Ruchała
Pharmacological Reports.2024; 76(1): 185. CrossRef - Increased risk of diabetes mellitus and hyperlipidemia in patients with differentiated thyroid cancer
Hwa Young Ahn, Jooyoung Lee, Jinmo Kang, Eun Kyung Lee
European Journal of Endocrinology.2024; 190(3): 248. CrossRef - Prevalencia de diabetes en personas con disfunción tiroidea
Juan J. Díez, Pedro Iglesias
Medicina Clínica.2023; 160(8): 333. CrossRef - Control of Thyroid Dysfunction in Spanish Population Registered in
the Primary Care Clinical Database: An Analysis of the Proportion of Patients
with Thyrotropin Values Outside the Reference Range
Juan J. Díez, Pedro Iglesias
Hormone and Metabolic Research.2023; 55(03): 184. CrossRef - Prevalence of thyroid dysfunction and its relationship to income level and employment status: a nationwide population-based study in Spain
Juan J. Díez, Pedro Iglesias
Hormones.2023; 22(2): 243. CrossRef - Prevalence of diabetes in people with thyroid dysfunction
Juan J. Díez, Pedro Iglesias
Medicina Clínica (English Edition).2023; 160(8): 333. CrossRef - Diabetes Mellitus Secondary to Endocrine Diseases: An Update of Diagnostic and Treatment Particularities
Mihaela Simona Popoviciu, Lorena Paduraru, Raluca Marinela Nutas, Alexandra Maria Ujoc, Galal Yahya, Kamel Metwally, Simona Cavalu
International Journal of Molecular Sciences.2023; 24(16): 12676. CrossRef - Thyroid Eye Disease and Its Association With Diabetes Mellitus: A Major Review
Roshmi Gupta, Pramila Kalra, Lakshmi B. Ramamurthy, Suryasnata Rath
Ophthalmic Plastic & Reconstructive Surgery.2023; 39(6S): S51. CrossRef - Metabolite Changes during the Transition from Hyperthyroidism to Euthyroidism in Patients with Graves’ Disease
Ho Yeop Lee, Byeong Chang Sim, Ha Thi Nga, Ji Sun Moon, Jingwen Tian, Nguyen Thi Linh, Sang Hyeon Ju, Dong Wook Choi, Daiki Setoyama, Hyon-Seung Yi
Endocrinology and Metabolism.2022; 37(6): 891. CrossRef - Diabetes and Hyperthyroidism: Is There a Causal Link?
Sang Yong Kim
Endocrinology and Metabolism.2021; 36(6): 1175. CrossRef
- Safety of non-standard regimen of systemic steroid therapy in patients with Graves’ orbitopathy: a single-centre experience

- Clinical Study
- Gender-Dependent Reference Range of Serum Calcitonin Levels in Healthy Korean Adults
- Eyun Song, Min Ji Jeon, Hye Jin Yoo, Sung Jin Bae, Tae Yong Kim, Won Bae Kim, Young Kee Shong, Hong-Kyu Kim, Won Gu Kim
- Endocrinol Metab. 2021;36(2):365-373. Published online April 7, 2021
- DOI: https://doi.org/10.3803/EnM.2020.939
- 5,015 View
- 152 Download
- 4 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Serum calcitonin measurement contains various clinical and methodological aspects. Its reference level is wide and unclear despite sensitive calcitonin kits are available. This study aimed to identify the specific reference range in the healthy Korean adults.
Methods
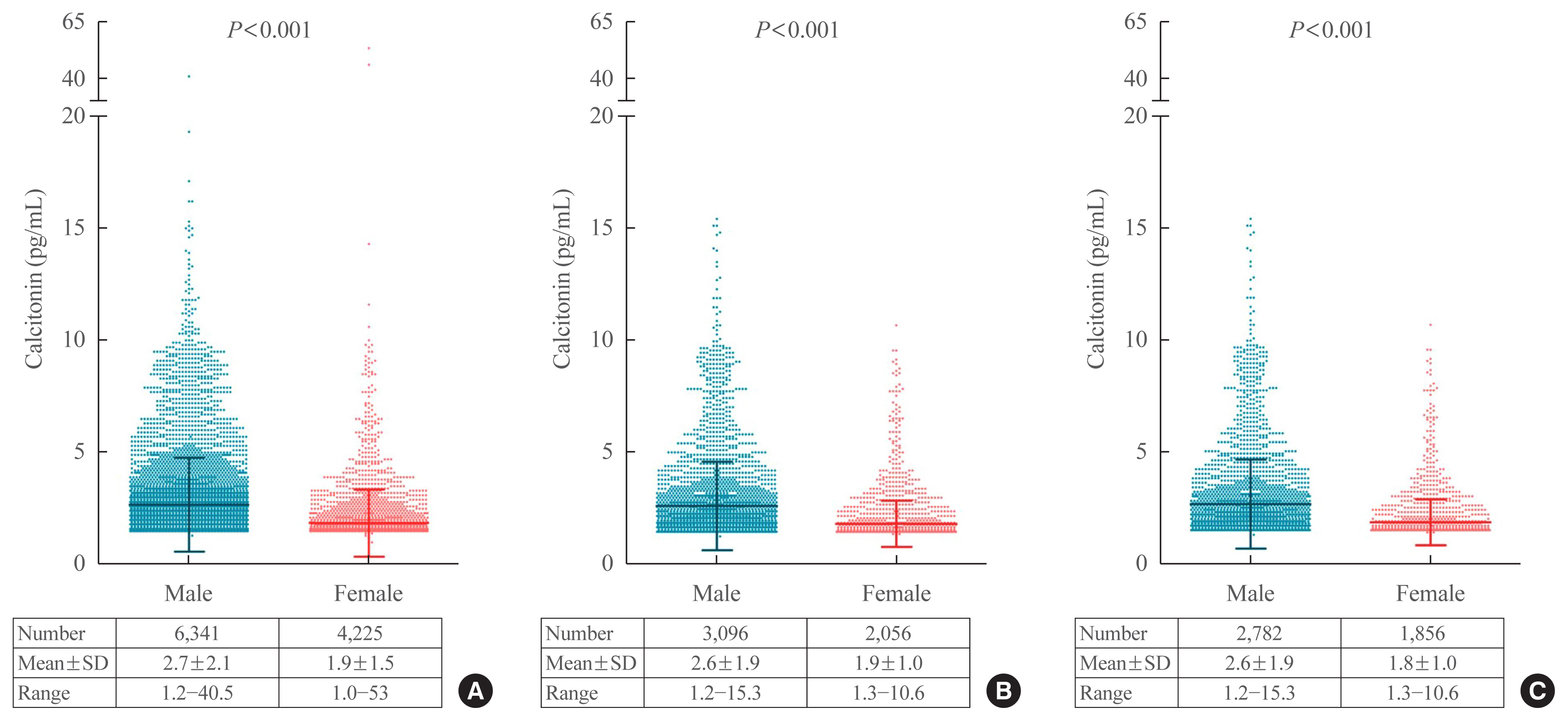
Subjects were ≥20 years with available calcitonin (measured by a two-site immunoradiometric assay) data by a routine health checkup. Three groups were defined as all eligible subjects (group 1, n=10,566); subjects without self or family history of thyroid disease (group 2, n=5,152); and subjects without chronic kidney disease, autoimmune thyroid disease, medication of proton pump inhibitor/H2 blocker/steroid, or other malignancies (group 3, n=4,638).
Results
This study included 6,341 male and 4,225 female subjects. Males had higher mean calcitonin than females (2.3 pg/mL vs. 1.9 pg/mL, P<0.001) in group 1. This gender difference remained similar in groups 2 and 3. Calcitonin according to age or body mass index was not significant in both genders. Higher calcitonin in smoking than nonsmoking men was observed but not in women. Sixty-nine subjects had calcitonin higher than the upper reference limit (10 pg/mL) and 64 of them had factors associated with hypercalcitoninemia besides medullary thyroid cancer. Our study suggests the reference intervals for men who were non, ex-, current smokers, and women (irrespective of smoking status) as <5.7, <7.1, <7.9, and <3.6 pg/mL, respectively.
Conclusion
Specific calcitonin reference range should be provided considering for sex and smoking status. Taking account for several factors known to induce hypercalcitoninemia can help interpret the gray zone of moderately elevated calcitonin. -
Citations
Citations to this article as recorded by- Determinants of circulating calcitonin value: analysis of thyroid features, demographic data, anthropometric characteristics, comorbidities, medications, and smoking habits in a population with histological full exclusion of medullary thyroid carcinoma
Pierpaolo Trimboli, Giuseppe Peloni, Dorotea Confalonieri, Elena Gamarra, Tommaso Piticchio, Francesco Frasca, Petra Makovac, Arnoldo Piccardo, Lorenzo Ruinelli
Frontiers in Oncology.2024;[Epub] CrossRef - Surgical treatment of solid variant of papillary thyroid carcinoma: Fifteen-year experience of a tertiary center
Katarina Tausanović, Marina Stojanović, Milan Jovanović, Boban Stepanović, Jovan Ilić, Sara Ivaniš, Vladan Živaljević
Medicinska istrazivanja.2024; 57(1): 121. CrossRef - Some genetic differences in patients with rheumatoid arthritis
Hosam M. Ahmad, Zaki M. Zaki, Asmaa S. Mohamed, Amr E. Ahmed
BMC Research Notes.2023;[Epub] CrossRef - Presence or severity of Hashimoto’s thyroiditis does not influence basal calcitonin levels: observations from CROHT biobank
M. Cvek, A. Punda, M. Brekalo, M. Plosnić, A. Barić, D. Kaličanin, L. Brčić, M. Vuletić, I. Gunjača, V. Torlak Lovrić, V. Škrabić, V. Boraska Perica
Journal of Endocrinological Investigation.2022; 45(3): 597. CrossRef - Environmental Factors That Affect Parathyroid Hormone and Calcitonin Levels
Mirjana Babić Leko, Nikolina Pleić, Ivana Gunjača, Tatijana Zemunik
International Journal of Molecular Sciences.2021; 23(1): 44. CrossRef
- Determinants of circulating calcitonin value: analysis of thyroid features, demographic data, anthropometric characteristics, comorbidities, medications, and smoking habits in a population with histological full exclusion of medullary thyroid carcinoma

- Clinical Study
- Impact of the Dynamic Change of Metabolic Health Status on the Incident Type 2 Diabetes: A Nationwide Population-Based Cohort Study
- Jung A Kim, Da Hye Kim, Seon Mee Kim, Yong Gyu Park, Nan Hee Kim, Sei Hyun Baik, Kyung Mook Choi, Kyungdo Han, Hye Jin Yoo
- Endocrinol Metab. 2019;34(4):406-414. Published online December 23, 2019
- DOI: https://doi.org/10.3803/EnM.2019.34.4.406
- 5,991 View
- 84 Download
- 16 Web of Science
- 19 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub Background Metabolically healthy obese (MHO) is regarded as a transient concept. We examined the effect of the dynamic change of metabolic health status on the incidence of type 2 diabetes mellitus (T2DM) both in obese and normal weight individuals.
Methods We analyzed 3,479,514 metabolically healthy subjects aged over 20 years from the Korean National Health Screening Program, who underwent health examination between 2009 and 2010, with a follow-up after 4 years. The relative risk for T2DM incidence until the December 2017 was compared among the four groups: stable metabolically healthy normal weight (MHNW), unstable MHNW, stable MHO, and unstable MHO.
Results During the 4 years, 11.1% of subjects in the MHNW group, and 31.5% in the MHO group converted to a metabolically unhealthy phenotype. In the multivariate adjusted model, the unstable MHO group showed the highest risk of T2DM (hazard ratio [HR], 4.67; 95% confidence interval [CI], 4.58 to 4.77). The unstable MHNW group had a higher risk of T2DM than stable MHO group ([HR, 3.23; 95% CI, 3.16 to 3.30] vs. [HR, 1.81; 95% CI, 1.76 to 1.85]). The stable MHO group showed a higher risk of T2DM than the stable MHNW group. The influence of the transition into a metabolically unhealthy phenotype on T2DM incidence was greater in subjects with aged <65 years, women, and those with weight gain.
Conclusion Metabolically healthy phenotype was transient both in normal weight and obese individuals. Maintaining metabolic health was critical for the prevention of T2DM, irrespective of their baseline body mass index.
-
Citations
Citations to this article as recorded by- Metabolically healthy obese individuals are still at high risk for diabetes: Application of the marginal structural model
Hye Ah Lee, Hyesook Park
Diabetes, Obesity and Metabolism.2024; 26(2): 431. CrossRef - Association of anthropometric parameters as a risk factor for development of diabetic retinopathy in patients with diabetes mellitus
Aditya Verma, Ashok Jha, Ahmed Roshdy Alagorie, Rishi Sharma
Eye.2023; 37(2): 303. CrossRef - From Metabolic Syndrome to Type 2 Diabetes in Youth
Dario Iafusco, Roberto Franceschi, Alice Maguolo, Salvatore Guercio Nuzio, Antonino Crinò, Maurizio Delvecchio, Lorenzo Iughetti, Claudio Maffeis, Valeria Calcaterra, Melania Manco
Children.2023; 10(3): 516. CrossRef - Assessment of Metabolic Syndrome Risk Based on Body Size Phenotype in Korean Adults: Analysis of Community-based Cohort Data
Ji Young Kim, Youngran Yang
Research in Community and Public Health Nursing.2023; 34: 158. CrossRef - Dynamic Changes in Metabolic Status Are Associated With Risk of Ocular Motor Cranial Nerve Palsies
Daye Diana Choi, Kyung-Ah Park, Kyungdo Han, Sei Yeul Oh
Journal of Neuro-Ophthalmology.2023;[Epub] CrossRef - New metabolic health definition might not be a reliable predictor for diabetes in the nonobese Chinese population
Liying Li, Ziqiong Wang, Haiyan Ruan, Muxin Zhang, Linxia Zhou, Xin Wei, Ye Zhu, Jiafu Wei, Xiaoping Chen, Sen He
Diabetes Research and Clinical Practice.2022; 184: 109213. CrossRef - Metabolically healthy obesity: Is it really healthy for type 2 diabetes mellitus?
Qi Wu, Ming-Feng Xia, Xin Gao
World Journal of Diabetes.2022; 13(2): 70. CrossRef - Metabolically obese phenotype and its dynamic change are associated with increased carotid intima-media thickness: Results from a cohort study
Liping Yang, Xue Li, Li Wang, Shan Xu, Yanmei Lou, Fulan Hu
Nutrition, Metabolism and Cardiovascular Diseases.2022; 32(9): 2238. CrossRef - Obesity Metabolic Phenotype, Changes in Time and Risk of Diabetes Mellitus in an Observational Prospective Study on General Population
Chan Yang, Xiaowei Liu, Yuanyuan Dang, Juan Li, Jingyun Jing, Di Tian, Jiangwei Qiu, Jiaxing Zhang, Ni Yan, Xiuying Liu, Yi Zhao, Yuhong Zhang
International Journal of Public Health.2022;[Epub] CrossRef - Implications of metabolic health status and obesity on the risk of kidney cancer: A nationwide population-based cohort study
Yun Kyung Cho, Hwi Seung Kim, Joong-Yeol Park, Woo Je Lee, Ye-Jee Kim, Chang Hee Jung
Frontiers in Endocrinology.2022;[Epub] CrossRef - Metabolic health is a determining factor for incident colorectal cancer in the obese population: A nationwide population‐based cohort study
Yun Kyung Cho, Jiwoo Lee, Hwi Seung Kim, Joong‐Yeol Park, Woo Je Lee, Ye‐Jee Kim, Chang Hee Jung
Cancer Medicine.2021; 10(1): 220. CrossRef - Cumulative Exposure to Metabolic Syndrome Components and the Risk of Dementia: A Nationwide Population-Based Study
Yunjung Cho, Kyungdo Han, Da Hye Kim, Yong-Moon Park, Kun-Ho Yoon, Mee Kyoung Kim, Seung-Hwan Lee
Endocrinology and Metabolism.2021; 36(2): 424. CrossRef - Excessive Intake of High-Fructose Corn Syrup Drinks Induces Impaired Glucose Tolerance
Hidemi Hattori, Yuma Hanai, Yuto Oshima, Hiroaki Kataoka, Nozomu Eto
Biomedicines.2021; 9(5): 541. CrossRef - The risk of Alzheimer’s disease according to dynamic changes in metabolic health and obesity: a nationwide population-based cohort study
Yun Kyung Cho, Jiwoo Lee, Hwi Seung Kim, Joong-Yeol Park, Woo Je Lee, Ye-Jee Kim, Chang Hee Jung
Aging.2021; 13(13): 16974. CrossRef - Metabolically healthy obesity: predictors of transformation to unhealthy phenotype in St Petersburg population (according to the ESSE-RF study)
M. A. Boyarinova, O. P. Rotar, A. M. Erina, N. A. Paskar, A. S. Alieva, E. V. Moguchaia, E. P. Kolesova, A. O. Konradi
"Arterial’naya Gipertenziya" ("Arterial Hypertension").2021; 27(3): 279. CrossRef - Physiological and Lifestyle Traits of Metabolic Dysfunction in the Absence of Obesity
Hanna Bjørk Klitgaard, Jesper Hoffmann Kilbak, Erica Arhnung Nozawa, Ann V. Seidel, Faidon Magkos
Current Diabetes Reports.2020;[Epub] CrossRef - Exploring Therapeutic Targets to Reverse or Prevent the Transition from Metabolically Healthy to Unhealthy Obesity
Tenzin D. Dagpo, Christopher J. Nolan, Viviane Delghingaro-Augusto
Cells.2020; 9(7): 1596. CrossRef - Prepregnancy smoking and the risk of gestational diabetes requiring insulin therapy
Mee Kyoung Kim, Kyungdo Han, Sang Youn You, Hyuk-Sang Kwon, Kun-Ho Yoon, Seung-Hwan Lee
Scientific Reports.2020;[Epub] CrossRef - Obesity with and without type 2 diabetes: are there differences in obesity history, lifestyle factors or concomitant pathology?
E. A. Shestakova, Yu. I. Yashkov, O. Yu. Rebrova, M. V. Kats, M. D. Samsonova, I. I. Dedov
Obesity and metabolism.2020; 17(4): 332. CrossRef
- Metabolically healthy obese individuals are still at high risk for diabetes: Application of the marginal structural model

- A Case of Multiple Osteoporotic Compression Fractures in Young Man with Budd-Chiari Syndrome.
- Sun Hwa Kim, Tae Un Yang, Byeong Kwang Choi, Hye Jin Yoo, Ji A Seo, Kyung Mook Choi, Nan Hee Kim, Sin Gon Kim, Sei Hyun Baik, Dong Seop Choi, Hae Yoon Choi
- Endocrinol Metab. 2012;27(4):334-339. Published online December 20, 2012
- DOI: https://doi.org/10.3803/EnM.2012.27.4.334
- 2,014 View
- 26 Download
-
 Abstract
Abstract
 PDF
PDF - Osteoporosis in young men is extremely rare. In this report, we demonstrate a rare case of multiple vertebral fractures discovered in a young man with Budd-Chiari syndrome without prior history of trauma. A 29-year-old man was diagnosed as Budd-Chiari syndrome 12 years ago and underwent a mesocaval shunt to relieve the hepatic vein obstruction and was on warfarin therapy. He suffered from low back pain and it was not relieved by analgesics. A T-L spine X-ray revealed multiple compression fractures and the z-score at lumbar spine was -3.7 which is below the expected range for that age. The patient was treated with calcium, vitamin D and bisphosphonate, and showed clinical improvement. This case highlights the importance of the investigation for secondary osteoporosis in young adults with an underlying disease that alters bone metabolism.

- Thyroid Dysfunction of North Korean Women Living in South Korea, Focusing on Subclinical Hypothyroidism.
- Joo Hyung Kim, Sol Ah Park, Nam Hoon Kim, Jae Hee Ahn, Yoon Jung Kim, Myongjin Cho, Yoon Jung Lee, Hye Jin Yoo, Hee Young Kim, Ji A Seo, Nan Hee Kim, Kyung Mook Choi, Sei Hyun Baik, Dong Seop Choi, Sin Gon Kim
- Endocrinol Metab. 2012;27(3):200-207. Published online September 19, 2012
- DOI: https://doi.org/10.3803/EnM.2012.27.3.200
- 3,510 View
- 27 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Thyroid function depends on ethnic and environmental factors. North Korean refugees have the same genetic background as South Koreans, but they have been exposed to different environments. This study examines the prevalence and pattern of thyroid disorders in North Korean women living in South Korea, focusing on subclinical hypothyroidism (SCH). METHODS: The intended sample was a total of 327 North Korean women residing in Seoul. Health questionnaires and medical examinations, including serum thyrotropin (thyroid stimulating hormone, TSH), free thyroxine, and thyroid autoantibodies, were conducted. RESULTS: The prevalence of SCH was 9.4%. In logistic regression analysis, smoking, menopause, length of stay in South Korea, body mass index, history of thyroid disease, and metabolic syndrome were not associated with the risk of SCH. Whereas, the positivity of autoantibodies were associated with a high risk for SCH (odds ratio [OR], 4.840; 95% confidence interval [CI], 1.80-13.017; P = 0.002), and age was associated with a low risk for SCH (OR, 0.94; 95% CI, 0.888-0.994; P = 0.031). The serum TSH levels also decreased with increasing age, and in particular, there was significant difference between 30-39 years, and over 60 years (2.33 +/- 1.51 microIU/mL vs. 1.54 +/- 0.73 microIU/mL, P = 0.028). CONCLUSION: In North Korean women, the positivity of autoantibodies was associated with a high risk for SCH. But interestingly, a younger age was associated with a high risk for SCH. Considering that they suffered from severe famine at the period of growth, and this led to malnutrition, their thyroid dysfunction might be associated with the peculiar environment that they experienced. -
Citations
Citations to this article as recorded by- Systematic review of evidence on public health in the Democratic People’s Republic of Korea
John J Park, Ah-Young Lim, Hyung-Soon Ahn, Andrew I Kim, Soyoung Choi, David HW Oh, Owen Lee-Park, Sharon Y Kim, Sun Jae Jung, Jesse B Bump, Rifat Atun, Hee Young Shin, Kee B Park
BMJ Global Health.2019; 4(2): e001133. CrossRef - Environmental Factors and Thyroid Dysfunction
Hyun-Kyung Chung
Endocrinology and Metabolism.2012; 27(3): 191. CrossRef
- Systematic review of evidence on public health in the Democratic People’s Republic of Korea

- Impact of the Serum Adiponectin Concentration on the Progression of Carotid Atherosclerosis in Patient with Type 2 Diabetes Mellitus.
- Hye Jin Yoo, Kyung Mook Choi
- Endocrinol Metab. 2012;27(1):28-30. Published online March 1, 2012
- DOI: https://doi.org/10.3803/EnM.2012.27.1.28
- 1,812 View
- 20 Download

- Hyperprolactinemia-Associated Breast Uptake of Radioiodine Following 131I Postablation Scan in Differentiated Thyroid Cancer.
- Jae Hee Ahn, Sun Young Kim, Ye Ji Kim, Suk Young Lee, Jae Hyoung Lee, Seung Hun Kang, Ho Cheol Hong, Sae Jeong Yang, Hye Jin Yoo, Ji A Seo, Sin Gon Kim, Nan Hee Kim, Kyung Mook Choi, Sei Hyun Baik, Dong Seop Choi, Hae Yoon Choi
- Endocrinol Metab. 2011;26(4):345-347. Published online December 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.4.345
- 1,955 View
- 22 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Scanning with whole-body 131I scintigraphy after surgery has been a valuable diagnostic modality in the surveillance of patients with differentiated thyroid cancer. Radioiodine uptake is rarely observed in non-lactating breast tissue, which mimics thyroid cancer metastasis. We now report a case of a 45-year-old female thyroid cancer patient who underwent radioiodine therapy, and in whom breast uptake of radioiodine was observed on a post-therapy whole body scan. Her serum prolactin level was elevated to 328 ng/mL at the time of the radioiodine uptake, and the hyperprolactinemia was induced by her antipsychotic medications. Six months after she discontinued that medication, her serum prolactin level was normalized to 12.6 ng/mL and breast uptake of iodine was no longer present in a follow-up whole body scan.
-
Citations
Citations to this article as recorded by- Incidental Findings of Intense Radioiodine Uptake in Struma Ovarii and Bilateral Nonlactating Breasts Simultaneously on Postablation 131I SPECT/CT for Papillary Thyroid Cancer
Hye-kyung Shim, Mi Ra Kim
Nuclear Medicine and Molecular Imaging.2016; 50(4): 353. CrossRef
- Incidental Findings of Intense Radioiodine Uptake in Struma Ovarii and Bilateral Nonlactating Breasts Simultaneously on Postablation 131I SPECT/CT for Papillary Thyroid Cancer

- Successful Localization of Distant Metastasis in Parathyroid Carcinoma Using Intraoperative Parathyroid Hormone Assay.
- Ho Cheol Hong, Sun Won Kim, Tae Hyung Kim, In Hye Cha, Jae Hee Ahn, Hye Jin Yoo, Hee Young Kim, Ji A Seo, Hyun Koo Kim, Sin Gon Kim, Nan Hee Kim, Kyung Mook Choi, Jae Bok Lee, Sei Hyun Baik, Dong Seop Choi
- Endocrinol Metab. 2011;26(1):92-96. Published online March 1, 2011
- DOI: https://doi.org/10.3803/EnM.2011.26.1.92
- 2,012 View
- 24 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Intra-operative parathyroid hormone (IOPTH) assay is a useful tool to confirm complete excision of all hyper-functioning parathyroid gland tissue. In this report, we describe a case with successful localization of distant metastasis in a patient with parathyroid carcinoma using the IOPTH assay. A 53-year-old man presented to our clinic with a serum calcium level of 11.8 mg/dL and an intact PTH level of 233.3 pg/mL. He had been treated for parathyroid carcinoma eleven years ago. Two suspected metastatic lesions were detected on the chest computed tomography. Due to the vastly different surgical field necessary to excise each lesion, we preferentially removed only one lesion and we monitored the other remaining suspected lesion without resection via IOPTH assay. Six months later, the patient's serum calcium and intact PTH levels remained within their normal ranges. To the best of our knowledge, this is the first case to effectively utilize IOPTH assay for the management of metastatic parathyroid carcinoma.
-
Citations
Citations to this article as recorded by- The association of abdominal obesity, obesity and parathyroid hormone in Korean adults (aged≥50 years): The Korea National Health and Nutrition Survey, 2011
Kyu Su Lee, Yo Sang Yoon, Hyun Yoon
Journal of the Korea Academia-Industrial cooperation Society.2015; 16(6): 3882. CrossRef
- The association of abdominal obesity, obesity and parathyroid hormone in Korean adults (aged≥50 years): The Korea National Health and Nutrition Survey, 2011

- Two Cases of Acromegaly with Empty Sella Syndrome Treated by Long-Acting Release Octreotide.
- Dong Jin Kim, Young Jin Seo, Nam Hoon Kim, Hye Soo Chung, Chai Ryoung Eun, Hye Jung Choi, Hye Sook Kim, Sae Jeong Yang, Juri Park, Hye Jin Yoo, Soo Yeon Park, Yun Jeong Lee, Ohk Hyun Ryu, Kye Won Lee, Hee Young Kim, Ji A Seo, Sin Gon Kim, Nan Hee Kim, Kyung Mook Choi, Sei Hyun Baik, Dong Seop Choi
- J Korean Endocr Soc. 2007;22(2):135-141. Published online April 1, 2007
- DOI: https://doi.org/10.3803/jkes.2007.22.2.135
- 2,008 View
- 27 Download
-
 Abstract
Abstract
 PDF
PDF - Two cases of typical acromegaly with empty sella syndrome presented to our institution. In the natural course of untreated pituitary adenoma, empty sella syndrome may result from necrosis by infarction or from hemorrhage of the pituitary gland. In our patients, the secretion of growth hormone continued in spite of the existence of empty sella syndrome. In one case, we confirmed the hypersecretion of growth hormone from sella by jugular vein sampling. Medical therapy with somatostatin analogue was attempted because there was no obvious mass in the sella. After 6~12 months of treatment with long-acting release octreotide, clinical features in our patients were improved, and the level of growth hormone and IGF-1 were also normalized.

- Comparison of Target Organ Damages between Primary Aldosteronism and Essential Hypertension.
- Juri Park, Dong Jin Kim, Sae Jeong Yang, Sook Hae Kim, Soo Yeon Park, Hye Jin Yoo, Yun Jeong Lee, Hee Young Kim, Ohk Hyun Ryu, Kye Won Lee, Ji A Seo, Sin Gon Kim, Kyung Mook Choi, Sei Hyun Baik, Dong Seop Choi
- J Korean Endocr Soc. 2007;22(1):11-18. Published online February 1, 2007
- DOI: https://doi.org/10.3803/jkes.2007.22.1.11
- 2,027 View
- 20 Download
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
A number of recent clinical studies have reported marked target organ damages in patients with primary aldosteronism. The aim of this study was to compare the incidence of target organ damages in patients with primary aldosteronism (PA) and essential hypertension (EHT). METHODS: The clinical records of 41 PA patients, over a 20-year period, were retrospectively analyzed. The clinical characteristics and incidence of target organ damages of 33 of the patients in this group were compared with those of 66 patients with essential hypertension, directly matched for age, gender and mean blood pressure. 8 of the PA patients could not be matched with EHT patients for age, gender and mean blood pressure, so were excluded from the comparison. The patients with essential hypertension were sampled from patients who visited for the evaluation of hypertension. RESULTS: Ischemic heart diseases were found in 18.2 and 10.6% of patients with PA and EHT, respectively (P = 0.22). From echocardiograms, left ventricular hypertrophy was found in 93.3% and 61.4% of patients with PA and EHT, respectively (P = 0.017). The degrees of left ventricular hypertrophy were correlated with the levels of serum aldosterone, with an r value of 0.490 (P < 0.005). Cerebrovascular attack was found in 18.2% and 1.5% of patients with PA and EHT, respectively (P = 0.005). Hypertensive retinopathy was found in 50% and 33.3% of patients with PA and EHT (P = 0.255), and nephropathy was found in 42.4% and 25.8% of patients with PA and EHT, respectively (P = 0.074). CONCLUSION: Patients with primary aldosteronism had target organ damages more frequently than with those with essential hypertension, which was independent of blood pressure. -
Citations
Citations to this article as recorded by- Changes in the clinical manifestations of primary aldosteronism
Sun Hwa Kim, Jae Hee Ahn, Ho Cheol Hong, Hae Yoon Choi, Yoon Jung Kim, Nam Hoon Kim, Hye Jin Yoo, Hee Young Kim, Ji A Seo, Nan Hee Kim, Sin Gon Kim, Kyung Mook Choi, Sei Hyun Baik, Dong Seop Choi
The Korean Journal of Internal Medicine.2014; 29(2): 217. CrossRef - Comparing the Prevalence of Primary Aldosteronism in Hypertensive Diabetic and Non-diabetic Patients
Yi Sun Jang, Koon Soon Kim, Hye Soo Kim
Journal of Korean Endocrine Society.2009; 24(4): 254. CrossRef - Aldosterone as a Cardiovascular Risk Factor
Soon Jib Yoo
Journal of Korean Endocrine Society.2007; 22(1): 8. CrossRef
- Changes in the clinical manifestations of primary aldosteronism

- A Case of Sheehan's Syndrome Presenting Central Diabetes Insipidus.
- Dong Jin Kim, Nan Hee Kim, Ju Ri Park, Sae Jeong Yang, Hye Suk Kim, Hye Jin Yoo, Soo Yeon Park, Ohk Hyun Ryu, Kye Won Lee, Hee Young Kim, Ji A Seo, Sin Gon Kim, Kyung Mook Choi, Sei Hyun Baik, Dong Seop Choi
- J Korean Endocr Soc. 2006;21(4):333-337. Published online August 1, 2006
- DOI: https://doi.org/10.3803/jkes.2006.21.4.333
- 2,057 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - Sheehan's syndrome occurs as a result of ischemic pituitary necrosis due to severe postpartum hemorrhage. The manifestations of this clinical syndrome are most often caused by a deficiency in the hormones produced by the anterior pituitary gland, whereas the neurohypophysis is usually preserved but can be involved in severe cases that manifest as diabetes insipidus. This is a report of Sheehan's syndrome that manifested with diabetes insipidus as presenting symptom 2 month's after delivery. The patient suffered massive bleeding, so received a blood transfusion. A combined pituitary stimulation and water deprivation test revealed deficiencies of not only anterior pituitary hormones, such as growth hormone and prolactin, but also of anti-diuretic hormone. We report this case, with a review of the literature.

- A Case of Primary Hyperparathyroidism Caused by Cystic Parathyroid Adenoma, Diagnosed during Intra-Operative PTH Monitoring.
- Hye Jin Yoo, Nan Hee Kim, Soo Yeon Park, Dong Jin Kim, Sae Jeung Yang, Ju Ri Park, Hee Young Kim, Ji A Seo, Kye Won Lee, Sin Gon Kim, Kyung Mook Choi, Jae Bok Lee, Young Seok Lee, Sei Hyun Baik, Dong Seop Choi
- J Korean Endocr Soc. 2005;20(3):278-282. Published online June 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.3.278
- 1,552 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - Primary hyperparathyroidism is the most frequent cause of hypercalcemia, and its prevalence is increasing due to the routine examination of serum calcium levels. Primary hyperparathyroidims is most commonly caused by an adenoma or hyperplasia of the parathyroid gland. A cystic parathyroid adenoma is an extremely rare cause of primary hyperparathyroidism. In our case, a-79-year old female presented with lower back pain and constipation. Her serum calcium, phosphate and immunoreactive parathyroid homone levels were 15.6, 1.8mg/dL and 371.8pg/mL, respectively. Neck CT revealed a cystic mass and a contour bulging heterogeneous mass in the left inferior right thyroid gland, respectively. These mass lesions were removed, and the intra-operative parathyroid hormone levels monitored, to confirm the complete resection. After removing the left cystic mass to the inferior thyroid, the serum calcium and immunoreactive parathyroid hormone levels quickly returned to normal. We report a case of primary hyperparathyroidism, caused by a cystic parathyroid adenoma, with a brief review of the literature


 KES
KES

 First
First Prev
Prev



